Congratulations to the REACH investigators listed below for their recent published work coming out of REACH!
- BACPAC REACH
- Feb 21, 2024
- 3 min read
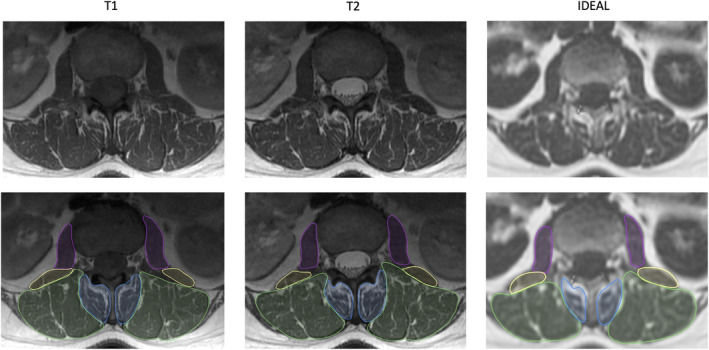
Postdoctor Scholar Dr. Noah Bonnheim and PI, Dr. Aaron Fields et al. published a paper titled "Deep-learning-based biomarker of spinal cartilage endplate health using ultra-short echo time magnetic resonance imaging". The causes of intervertebral disc degeneration, which may cause chronic low back pain in some individuals, are not completely understood. Recent studies have emphasized the significance of the cartilage endplate in disc health, yet the clinical impact of these discoveries is limited by an inability to assess the cartilage endplate in patients. Here, we sought to facilitate the development and clinical translation of MRI-based biomarkers of cartilage endplate composition to provide diagnostic tools for assessing cartilage endplate health in patients. To do this, we used ultra-short echo time magnetic resonance imaging (UTE MRI) to generate T2* maps of the endplate, which provide non-invasive spatial assays of endplate composition. Then, we trained deep learning models to automatically segment the cartilage endplate using UTE images to facilitate objective, accurate, and efficient biomarker analysis. Our findings show that, compared to manual techniques, our models' segmentations allow for the stratification of cartilage endplates into diagnostic subgroups with high sensitivity (0.77–0.86) and specificity (0.86–0.95). Demonstrating the applicability of our results, model performance was consistent across different MRI machines and linked to image quality factors like signal- and contrast-to-noise ratios. The imaging biomarkers and software tools we've developed support the evaluation of cartilage endplate health in individuals with chronic low back pain. We're now applying these methods to explore the cartilage endplate's role in disc degeneration and understand treatment outcomes following intradiscal biologic therapy for disc regeneration.
Read the full article in Quantitative Imaging in Medicine and Surgery (QIMS) here.

Dr. Leslie Wilson et al. published a paper titled "Preferences for Risks and Benefits of Treatment Outcomes for Chronic Low Back Pain: Choice-Based Conjoint Measure Development and Discrete Choice Experiment". Understanding individual patient preferences for chronic low back pain (cLBP) outcomes is essential for targeting available therapeutic options; yet tools to elicit patient outcome preferences are limited. Our objective was to develop and test a choice-based conjoint (CBC) measure, commonly used in behavioral economics research, to elicit what outcomes patients with cLBP want to achieve and avoid. We developed a survey-based CBC measure to allow patients to make risk/benefit trade-off choices between possible treatment outcomes. After extensive literature, clinician, and patient input, our measure included seven attributes: fatigue, anxiety/depression, difficulty thinking/making decisions, pain intensity, physical abilities, change in pain, and ability to enjoy life despite pain. Random-parameters logit models were used to estimate strength of preferences, and latent class analysis was used to identify patient characteristics associated with distinct preference. This was an online study using the Sawtooth web-based platform to collect data. Two hundred eleven individuals with cLBP were recruited from online advertising as well as at clinical sites across multiple academic and private institutions.
Our results showed that the most valued outcome was the highest level of physical activity (β = 1.6-1.98; p < .001), followed by avoiding cognitive difficulties (β = -1.48; p < .001). Avoidance of severe pain was comparable to avoiding constant fatigue and near-constant depression/anxiety (β = -0.99, -1.02); p < .001). There was an association between preferences and current pain/disability status; patients with higher pain had a stronger preference to avoid severe pain, whereas those with higher disability have stronger preferences for achieving physical activity. The latent class analysis identified two distinct groups: (1) more risk-seeking and willing to accept worse outcomes (56%); and (2) more risk-averse with a stronger preference for achieving maximum benefits (44%).
In conclusion, our study illuminated cLBP patient preferences for treatment outcomes and heterogeneity in these preferences. Patients stressed the importance of reaching high physical activity and avoiding cognitive declines, even over a desire to avoid pain. More work is needed to understand patient preferences to aid informed, shared decisions.
Read the full article in Physical Medicine and Rehabilitation (PM&R) here.

Figure: CAPER outcomes.


Comments